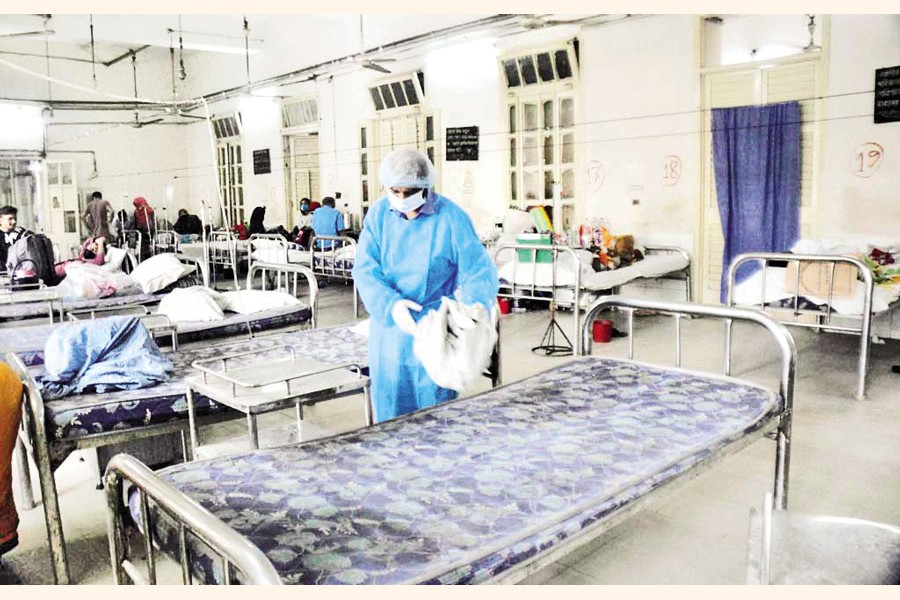
 Out of a total of 616 public hospitals and medical colleges across the country, 136 are in Dhaka and 129 in Chattogram with the two cities accounting for 43 per cent of the total
Out of a total of 616 public hospitals and medical colleges across the country, 136 are in Dhaka and 129 in Chattogram with the two cities accounting for 43 per cent of the total  As the new coronavirus spreads globally, tragic human consequences and socioeconomic losses at various levels are rapidly unfolding. Alongside direct disastrous impact on health, the pandemic does have indirect impact on environment, livelihoods and supply chains that has made the rebound of economies like Bangladesh tougher.
As the new coronavirus spreads globally, tragic human consequences and socioeconomic losses at various levels are rapidly unfolding. Alongside direct disastrous impact on health, the pandemic does have indirect impact on environment, livelihoods and supply chains that has made the rebound of economies like Bangladesh tougher.
Soon after the first reported case of the viral disease on March 08 last, the issue involving the capacity of the health sector has come to the fore. The sector has long been struggling to serve both urban and rural patients equally because of its highly centralised policy. The result has been obvious, a robust inequality has surfaced, resulting in untimely death of many and putting health of millions of others at risk.
The issue of health inequality, the outcome of a disproportionate allocation of health related resources, came to light recently as many corona patients for lack of oxygen, ICUs, testing facilities and proper treatment died in different parts of the country. The Financial Express (FE) recently published a series of reports over disparity in the health management system across the country.
Before finding solutions to the inequality, we can have a look at the division-wise statistics of the available services across the country. According to the FE reports that have cited DGHS data, the country has a total of 616 public hospitals and medical colleges.
Of which 43 per cent or 265 are concentrated in Dhaka (136) and Chattogram. The numbers are only 36, 46, 52, 66, 69 and 82 in Mymensingh, Sylhet, Barisal, Rangpur, Khulna and Rajshahi respectively. Regarding the private hospitals or clinics, Dhaka and Chattogram accounted for half of the country's 17244 private healthcare facilities.
In terms of doctors, there are 26310 government physicians and 57.35 per cent and 11.56 per cent posted in Dhaka and Chattogram respectively. Half of the government-recruited nurses are working in these two mega cities while the figure is almost the same as far as number of technicians are concerned. The disparity is more severe in the case of fighting the COVID-19 pandemic as all 30 covid-dedicatd hospitals are located in Dhaka (21) and Chattogram (9). In testing lab facilities for detecting coronavirus infections, 63 out of 92 PCR labs located in Dhaka followed by 13 in Chattogram while others divisions do have two or three labs.
The situation turned worse during the first four to five months of the pandemic as a good number of healthcare professionals skipped their duties in fear of infection. In fact, many healthcare facilities stopped providing the services that created a crisis situation for thousands of non-Covid patients .
Along with challenges, each disaster creates opportunities. The Covid-19 also has done so for Bangladesh exposing the lacking in the service delivery at all levels. The policymakers must take lessons from the Covid-19 pandemic and equip the facilities in a way so that it can respond more efficiently when the next outbreak comes. For achieving this target, focus should be given immediately on decentralisation of resources by empowering the local governments. The holistic change in the policies must come from the level of budget formulation and will end with need-based distribution of human resources. We also need to make prudent investment in the health sector keeping demand for the service from the population of a particular area into consideration. This is because the current practice of the budget disbursement is not only faulty but also skewed.
Currently, the government used to make budgetary allocation based on the capacity of local public healthcare facilities but the capacity of these facilities is not created in accordance with the need of the population. We need to build capacity of our hospitals taking into consideration the population size of particular localities and make budgetary allocations accordingly. Then it will make sense. Otherwise, we cannot narrow the ever- widening disparity.
Another key health infrastructure issue that has not been widely discussed yet is the absence of central oxygen storage facilities even in large government health facilities. The government keeps building medical college and hospitals in various parts of the country but most of them do not have central oxygen storage facilities that are much more efficient than transporting oxygen in compressed gas cylinders. A longer-term solution for the hospitals is to build their own oxygen plants. It can cost from Tk 100 million to Tk 200 million but investing can ensure oxygen access across a large area.
Another major problem that the sector faces is apathy of the healthcare professionals to get engaged in the rural areas. The time has come to incentivise the professionals in a way that will help allure them going to the rural health centres. The authorities of the medical colleges can encourage medical students of the least developed regions giving them additional marks in the exams on condition that they will be serving people in primary, secondary and tertiary level in these regions and they cannot apply for going to other districts. The government can also make it mandatory for students that those who will study district-level medical colleges will be serving there. We can look for these options for a certain time until it is saturated. The decision on this matter must come from the high-ups of the government and it must be approved by the parliament.
Although the pandemic has been causing severe public health and economic disruptions all over the world, a few countries have been successful in dealing with the virus. For example, China, from where the virus reportedly originated, Singapore, South Korea and Japan have done well in containing the virus. China taught the whole world the importance of preparedness to prevent and control infectious disease outbreak with the use of technology while the South Korean approach for isolating the infected patients and building awareness among the people through the social media platforms. On the other hand, the main focus of Singapore was to track the virus-affected people and isolate the virus-free people from the affected ones by keeping the latter in hospital until they recover. We need to know more how they became successful. What were their strategies or priorities. We should arrange regular discussion with policymakers and medical staff of these countries so that we can also replicate these to stem the pandemic from spreading.
Alongside reforms in the healthcare sector, Bangladesh requires to pay serious attention to vaccine diplomacy maintaining contact with all the potential vaccine-producing countries. However, it will still be too premature to make any final procurement deal with any potential vaccine-producing country right now since it is not clear which vaccine may prove safe and effective on completion of its phase-III trial. Taking the country's overall vaccine-related activities into consideration, Bangladesh seems lagging behind in corona vaccine diplomacy for lack of proper planning, strategy and initiative. We need smart and effective diplomacy with proper planning and strategy to have enough doses of vaccine. It will not be a wise decision to have a vaccine relying only on bilateral relations with a few countries. Economic diplomacy is also very important here. Bangladesh with its large population is surely a big market for the vaccine producers which can be used as a bargaining tool during the negotiation. Two economic powerhouses -- China and India - in the region have already assured Bangladesh of giving priority in providing their vaccines once those are ready. But these countries will have huge internal demand due to their large population size. We need to focus on getting permission for manufacturing any vaccine in our country to ensure its availability here in due time. Simultaneously, attention needs to be paid on the possible homegrown vaccine initiative.
We need to learn the lessons that this pandemic has taught us for months and prepare our disease-tackling units investing sufficient resources in them. We should not forget that this pandemic is not the last one. But before the next pandemic comes, we must be ready to deal with it efficiently.
The writer is a Senior Reporter of the FE.
jubairfe1980@gmail.com
© 2026 - All Rights with The Financial Express
