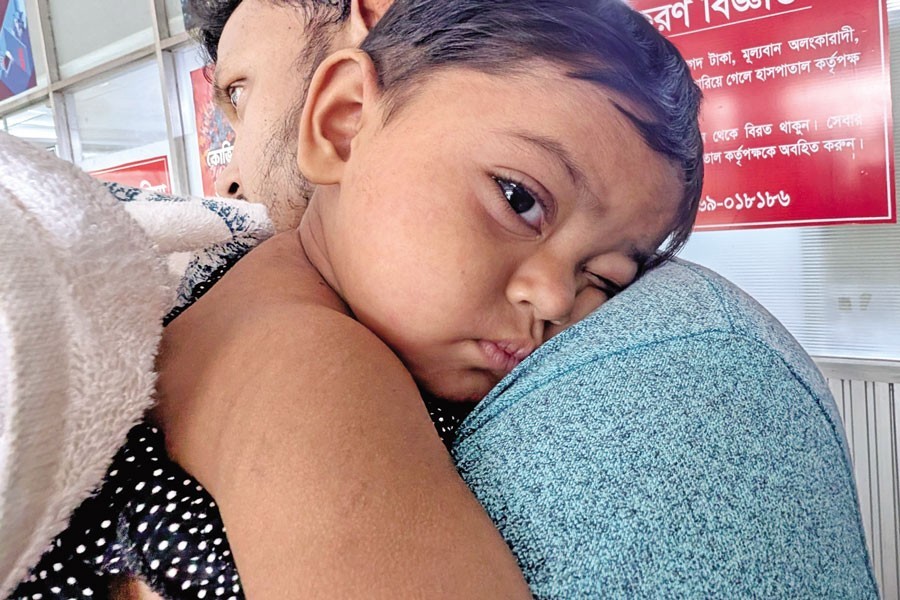
 A measles-infected child rests on his father's shoulder as they wait to seek treatment at DNCC Covid Hospital in the city, which is now admitting only patients with measles or measles-like symptoms —FE file photo
A measles-infected child rests on his father's shoulder as they wait to seek treatment at DNCC Covid Hospital in the city, which is now admitting only patients with measles or measles-like symptoms —FE file photo The deaths are real, the causes are complex, and the solutions are largely known. What is needed now is honesty, not about who to blame, but about what needs to change.
Bangladesh is grieving. Many children have died of measles in recent weeks, and many more remain in hospital. The scale of this tragedy cannot be captured by case counts alone. The right questions are not just "how many," but "who is dying, and why?" And what does careful, honest analysis tell us about what needs to change?
WHAT THE DATA SHOWS: The latest official and publicly available data is stark. The World Health Organisation reported that between March 15 and April 13, 2026, Bangladesh recorded 19,161 suspected measles cases across 58 of 64 districts, including 2,973 laboratory-confirmed infections. There were 166 suspected deaths, of which 30 were confirmed, and more than 12,000 hospital admissions in a single month. The burden has fallen overwhelmingly on young children. Seventy-nine per cent of cases were in children under five, and one-third were infants under nine months, too young to complete the full vaccination schedule. Among confirmed cases, nearly three-quarters had not received even a single dose of the measles vaccine.
More recent government data reported on May 4 suggests that the situation has worsened. Suspected cases have risen to over 41,000, and 311 children have died since March, including 17 deaths in a single day, the highest recorded so far. In Dhaka, cases are concentrated in densely populated informal settlements such as Demra, Jatrabari, Kamrangirchar, Korail, Mirpur, and Tejgaon. This is not accidental. The virus finds unvaccinated children, and these are often the very children the health system has struggled to reach. These numbers are not just statistics. They reflect patterns of vulnerability that have been building for some time.
MEASLES AS A TRIGGER, NOT THE PRIMARY CAUSE: Measles is one of the most contagious viral diseases known. A single case can infect up to 18 unvaccinated people. Yet it rarely kills directly. Most deaths occur through complications such as pneumonia, severe diarrhoea, or respiratory distress.
In that sense, measles is often a trigger rather than the primary cause. It exposes underlying weaknesses, both in children's health and in the systems meant to protect them. Where children are well nourished, vaccinated, and able to access care quickly, survival is usually the outcome. Where those conditions are missing, the risks rise sharply.
This distinction matters. When deaths increase during a measles outbreak, it tells us two things at once. It shows who was left unprotected before the outbreak began, and how well the system is able to respond once it does.
WHO IS MOST AT RISK AND WHY: The children who are dying are overwhelmingly those who were never vaccinated and those already weakened by malnutrition. In Bangladesh, approximately 24 per cent of children under five are stunted, according to the latest national data. This is not just a development indicator. It is a marker of vulnerability. A malnourished child has a weaker immune response, and infections that would otherwise be manageable can become life threatening. This is why deaths are concentrated among the poorest households. The issue is not only exposure to the virus, but the conditions children live in long before they encounter it.
Vaccination data tell a similar story. Even before the outbreak, coverage had begun to slip. First dose measles rubella coverage declined from 88.6 percent to 86 percent between 2019 and 2024. Second dose coverage fell more sharply, from 89 percent to 80.7 percent. That translates into millions of children without full protection. With a disease as infectious as measles, even small gaps can have large consequences.
Vitamin A is another critical factor that often receives less attention. Evidence shows that timely supplementation can significantly reduce the risk of death, by as much as half in populations where deficiency is common, according to WHO. It is inexpensive and widely available. Yet recent disruptions mean that several distribution campaigns have been missed. This is not a minor issue. It is a gap that can be closed quickly and one that can save lives.
Does reaching a hospital ensure survival: Reaching a hospital does not always guarantee survival. Severe measles requires timely treatment of complications. Pneumonia must be treated with antibiotics. Dehydration must be managed with fluids. Children with breathing difficulties need oxygen and close monitoring.
When these are available in time, children recover. But when hospitals are overcrowded, when families arrive late, or when supplies are stretched, outcomes worsen. Reports from across the country suggest that isolation units are operating far beyond their intended capacity. This does not mean the virus has become more dangerous. It means the system is under strain. It is also important to recognise that many deaths occur before children reach care, at home, on the way to hospital, or after being turned away from overcrowded facilities. The official numbers are therefore likely to underestimate the true scale of loss.
THE COVID INHERITANCE: No account of the current situation is complete without looking at the COVID-19 period. Between 2020 and 2022, routine immunisation systems were disrupted around the world. According to the UNICEF, about 25 million children missed routine vaccinations in 2021 alone, the largest setback in decades.
Bangladesh was not spared. Children who missed vaccines during those years did not automatically return to the system once the pandemic eased. They needed to be identified and reached. Where that did not happen, vulnerability built quietly over time.
Plans for a nationwide measles rubella campaign in 2024 were postponed and eventually cancelled. As a result, several groups of children remained unprotected. These accumulated gaps created the conditions for the outbreak we are now seeing.
There are also concerns about vaccine supply in 2024 and 2025. Government data has suggested a sharp drop in coverage during this period, though this needs clearer public explanation from authorities. The most reasonable conclusion is that risk built up over several years and recent disruptions pushed it into a crisis.
THIS IS NOT ONLY A BANGLADESH STORY: Before drawing narrow conclusions, it is important to place this outbreak in a wider context. Measles is resurging globally. According to the World Health Organization, millions of cases continue to occur each year, mostly among unvaccinated children. Countries that had previously eliminated measles are now seeing it return. The United States has recorded a sharp rise in cases. Parts of Europe have lost elimination status. Across several regions, outbreaks have followed the same pattern.
The causes are also similar. COVID disruptions left many children without vaccines. In some places, hesitancy has grown. In others, inequalities in access have persisted. Even strong health systems can fail specific communities when coverage drops in particular areas.
This perspective matters. Bangladesh's situation is part of a global trend, but it also reflects local gaps. Recognising both is essential for an effective response.
A recent ScienceInsider article has been widely shared in discussions of the outbreak. It offers a plausible narrative, but it is not based on peer reviewed research, and a sequence of events does not, on its own, establish causation. The evidence points instead to a gradual accumulation of risk. Simplifying that story too much does not help. Ignoring recent weaknesses does not help either.
WHAT NEEDS TO BE DONE NOW: The first priority is to restore immunisation as a core national commitment. Routine services need to be strengthened, and catch up efforts must be expanded. Children who missed vaccines during the pandemic years need to be actively found and protected. Campaigns that are now underway are important, but they must reach every community where gaps remain.
The second priority is to prepare the health system. Hospitals need the capacity, staff, and supplies to manage severe cases. This means planning ahead rather than responding under pressure. Simple interventions, including Vitamin A supplementation, must be available everywhere measles is treated.
The third priority is to focus on the children who are hardest to reach. National averages can hide the problem. The outbreak is concentrated in communities that are often overlooked. Reaching them requires careful planning, local engagement, and consistent follow up.
THE PATH FORWARD: Measles reveals weaknesses that are often hidden. It shows where systems are not reaching those who need them most. The current outbreak is a tragedy, but it is also a signal. Bangladesh has made remarkable progress in public health over the past decades. That progress is real and should not be dismissed. But it cannot be taken for granted. It requires constant attention, especially after disruptions like a global pandemic.
The virus does not distinguish between countries. It spreads wherever immunity is weak. The response must therefore be consistent. Every child must be reached. Every gap must be closed.
Children are dying today not because measles cannot be controlled, but because vulnerabilities were allowed to build. Recognising that is not about assigning blame. It is about making sure those gaps are closed before the next outbreak begins.
Asad Islam is Professor of Economics at Monash Business School, Monash University, and conducts research on public health issues in Bangladesh and other developing countries.
© 2026 - All Rights with The Financial Express
